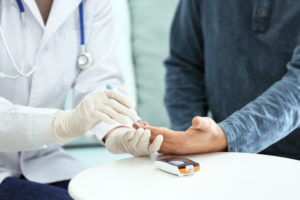
Gestational diabetes is a form diabetes that is first recognized in pregnancy. Gestational diabetes occurs because the mother’s pancreas does not make enough extra insulin to control the blood sugar needed when hormones from the placenta block the normal action of insulin. These hormones rise most in the second part of pregnancy and so this is when gestational diabetes is typically found.
In gestational diabetes, the major concern is that the higher blood sugar levels cross the placenta into the baby, and the baby converts the sugar into fat. These babies may get too big, making for a more difficult delivery. Also, the baby may get used to higher sugars and so just after birth the baby’s blood sugar may drop and they can have low blood sugar (hypoglycemia). We have never seen a baby born with diabetes because the mom had gestational diabetes.
For the mother, gestational diabetes usually resolves once the baby is born. Because the mother’s pancreas is now known to need a little help, women who had gestational diabetes are at higher risk for the development of type 2 diabetes later in life, a risk that can be reduced by adopting healthy eating and physical activity habits.
Most cases of gestational diabetes respond very well to eating healthy food and activity. Walking after meals helps use up blood sugar and keeps it controlled. About one third of women may need insulin/blood sugar lowering medications even with healthy eating habits and exercising. Medications taken during pregnancy for GDM can nearly always be stopped once the baby is born.
Why Me? Why Now?
At this point you may or may not have been told by your healthcare provider that you have gestational diabetes. You are probably wondering why me?
The short answer is that it can happen to any woman and gestational diabetes is different from regular diabetes in that it simply means your body is having trouble managing your blood sugar levels during your pregnancy.
“Hang On A Minute, I’ve Already Attended My Gestational Diabetes Class!”
Great! That means that you have been given the tools and advice that you need to manage your gestational diabetes. It is important that you follow your health care providers’ recommendations which may include recording what you eat, when you exercise, and what your blood sugar levels are. We know that for many of you this may feel like a lot of work, while some of you may find that you are already eating healthy with the right amount of activity. In any case, keeping records, testing blood sugar levels, and preparing healthy meals may take some getting used to. Be sure to call your health care team if you are unsure about your choices or the recommendations.
The Hard Truths: GDM Risk Factors
Age:
As women get older, the risk of GDM increases. Being over 35 increases your risk.
Ethnicity:
Women who are Indigenous, Asian, Hispanic, and others are at higher risk for developing gestational diabetes.
Weight:
Being overweight before you become pregnant and/or excess weight gain during pregnancy can increase your risk for developing gestational diabetes. Your health care provider can give you some guidance on how much weight you should be gaining for your pregnancy. Learn more.
Previous pregnancies with gestational diabetes:
If you had gestational diabetes in a previous pregnancy, you are more likely to develop it in a later pregnancy. If you previously had a large-at-birth baby, this can also be a clue you’re at risk of developing gestational diabetes.
But wait – I don’t have any of these risk factors! Could my health care team be wrong?
Unfortunately, many women without any known risk factors develop gestational diabetes. This is why Diabetes Canada (and most Diabetes guidelines world-wide) recommend that all women should be screened for gestational diabetes no later than 28 weeks’ gestation in their first pregnancy, and earlier in subsequent pregnancies if they had GDM before.
What Happens To My Baby While I Am Pregnant??
Ever hear of the old saying, “you are what you eat?” The saying holds true in gestational diabetes because the foods you eat that are high in sugar not only affect your blood sugar levels but also your baby.
Babies born to moms with uncontrolled high blood sugar levels are more prone to store that sugar as fat, leading to a larger baby at birth which can create difficulties during delivery.
In Alberta, having gestational diabetes doubles your chance of having a larger baby so it is important to follow the nutritional and medical guidance of your health care team.
What About Baby Feeding?
It is safe and encouraged to breastfeed after having GDM, but if your blood sugars remain high after delivery and you still require medications, please consult with your doctor and lactation consultant.
What Happens To Blood Sugar Levels After Delivery In My Baby And I?”
Having diabetes in pregnancy may expose your baby to higher blood sugar during your pregnancy. Once the baby and placenta are delivered, the hormones that cause diabetes in pregnancy drop quickly resulting in lower blood sugars in you. Most of the time your blood sugar levels will return to normal after pregnancy (and if you needed insulin during the pregnancy you will likely no longer need it!) Hooray!
If the baby has been exposed to high blood sugars throughout pregnancy, there is a chance the baby’s blood sugar may go low after delivery although this is rare in gestational diabetes and found more frequently in pre-existing diabetes.